What is Psoriasis?
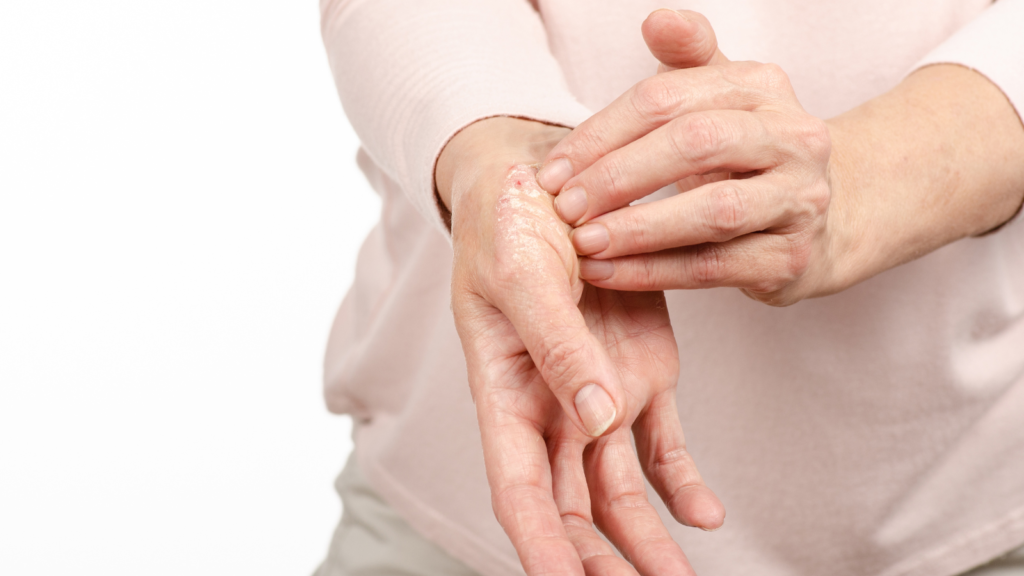
Psoriasis is a chronic autoimmune skin disorder characterized by the rapid growth of skin cells, leading to the formation of thick, red, and scaly patches on the skin. It is a non-contagious condition that affects approximately 2-3% of the global population. Psoriasis can occur on any part of the body, but it commonly appears on the elbows, knees, scalp, lower back, and nails.
Type of Psoriasis?
Jaundice can be classified into three main types, based on the underlying cause:
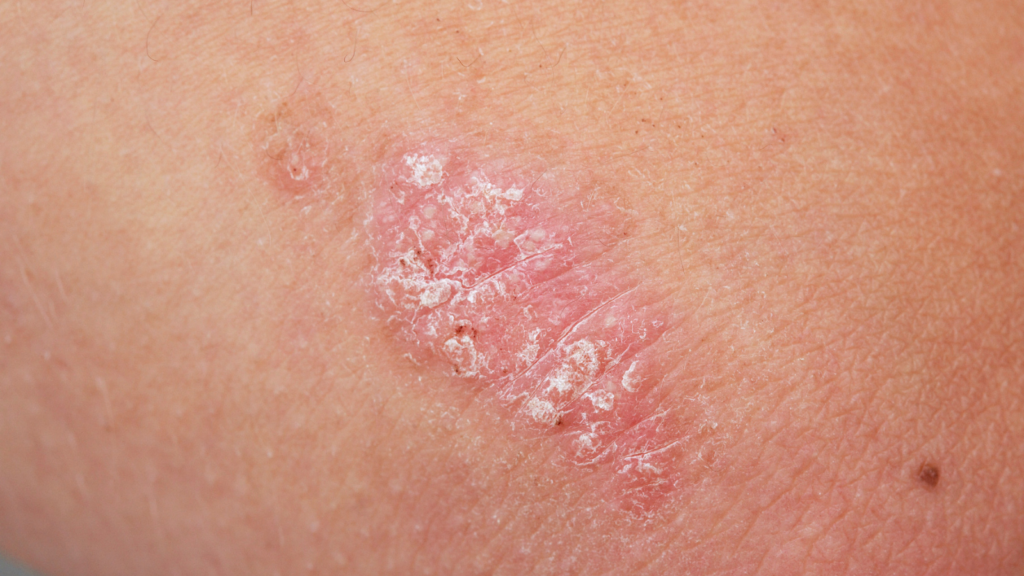
Plaque Psoriasis
The most common form of psoriasis, characterized by raised, red patches covered with a silvery-white buildup of dead skin cells (scale).
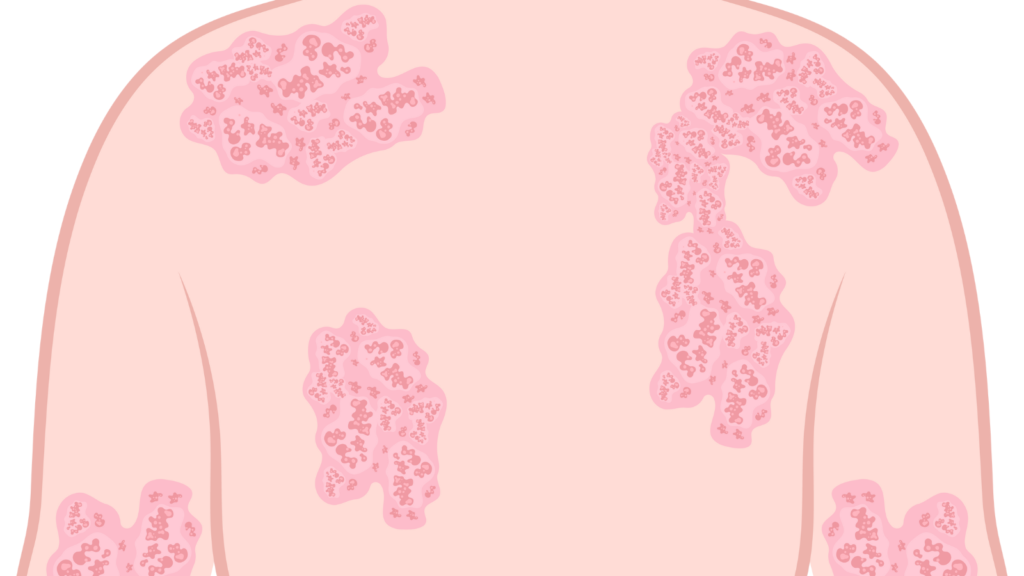
Guttate Psoriasis
Characterized by small, drop-shaped lesions that often appear suddenly, usually triggered by bacterial or viral infections, such as strep throat.
Inverse Psoriasis
Occurs in skin folds, such as the armpits, groin, or under the breasts, where it appears as smooth, red patches without the typical scaling seen in other types of psoriasis.
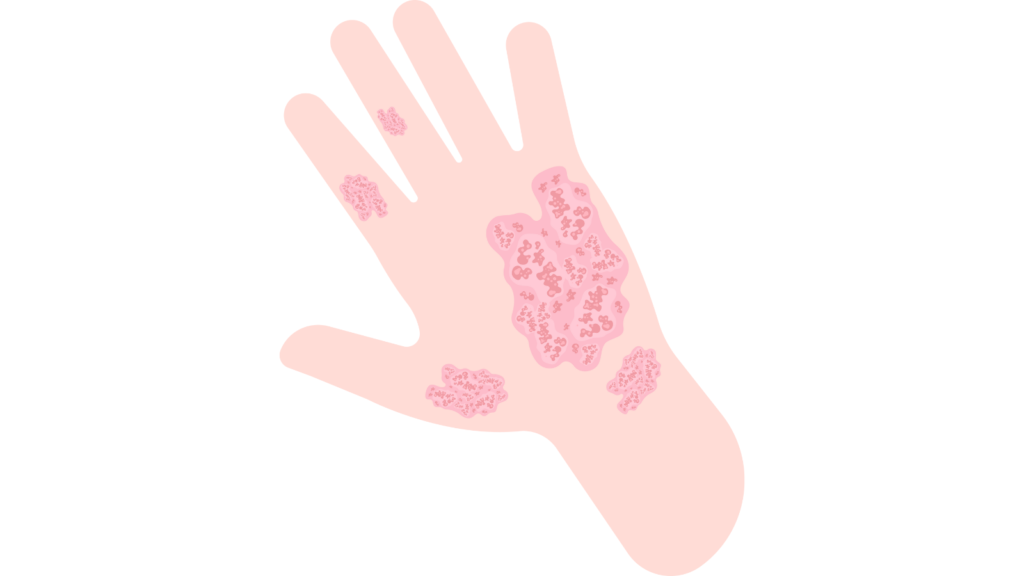
Pustular Psoriasis
Characterized by the appearance of pus-filled blisters (pustules) surrounded by red skin. It can be localized to specific areas of the body or generalized, covering large areas.
Erythrodermic Psoriasis
A rare and severe form of psoriasis that can cover the entire body with a red, peeling rash that resembles severe burns. It can cause intense itching, pain, and complications such as dehydration and infection.

What are the symptoms of Psoriasis?
Psoriasis symptoms can vary depending on the type of psoriasis and its severity. Common symptoms of psoriasis include:
Red Patches of Skin
Psoriasis typically presents as raised, red patches of skin, known as plaques. These patches may vary in size and can appear anywhere on the body, but they are most commonly found on the elbows, knees, scalp, lower back, and nails.
Thickened Skin
The skin affected by psoriasis may become thickened, particularly over the plaques. This thickening can give the skin a rough or scaly texture.
Silvery-White Scales
Over the red patches of skin, psoriasis often produces silvery-white scales or plaques. These scales are made up of dead skin cells that accumulate as a result of the rapid turnover of skin cells in psoriasis.
Itching and Irritation
Psoriasis plaques can be itchy and may cause irritation or discomfort, especially if they crack or bleed.
Dry, Cracked Skin
Psoriasis can cause the skin to become dry and prone to cracking, particularly in areas where plaques form, such as elbows and knees.
Bleeding
In severe cases or if scratching is excessive, psoriasis plaques may bleed.
Nail Changes
Psoriasis can affect the nails, causing changes such as pitting (small dents or depressions), thickening, discoloration, crumbling, or separation of the nail from the nail bed.
Joint Pain and Swelling
Some individuals with psoriasis, particularly those with psoriatic arthritis, may experience joint pain, swelling, and stiffness. Psoriatic arthritis can affect any joint in the body, but it most commonly affects the joints of the fingers and toes.
Scalp Psoriasis Symptoms
When psoriasis affects the scalp, symptoms may include red patches, scaling, itching, and in severe cases, hair loss.
Inverse Psoriasis Symptoms
Inverse psoriasis, which occurs in skin folds such as the armpits, groin, or under the breasts, may present as smooth, red patches without scaling. It may also cause discomfort or irritation due to the moist environment of skin folds.
What are the causes of Psoriasis?
The exact cause of psoriasis is not fully understood, but it is believed to involve a combination of genetic, immune system, and environmental factors. Some of the key factors thought to contribute to the development of psoriasis include:
Genetic Predisposition
Psoriasis tends to run in families, suggesting a genetic component to the condition. Certain genetic variations (mutations) may increase susceptibility to psoriasis by affecting immune system function and skin cell growth.
Immune System Dysfunction
Psoriasis is considered an autoimmune disorder, in which the body’s immune system mistakenly attacks healthy skin cells, triggering inflammation and causing the rapid growth of skin cells. T cells, a type of white blood cell involved in immune responses, play a key role in the immune system dysfunction seen in psoriasis.
Environmental Triggers
Various environmental factors, such as infections, injury to the skin, stress, certain medications, and hormonal changes, can trigger or exacerbate psoriasis symptoms in susceptible individuals. Common triggers include respiratory infections (e.g., streptococcal infections), skin injuries (e.g., cuts, scrapes, sunburns), stress, and certain medications (e.g., lithium, beta-blockers, antimalarial drugs).
Inflammatory Pathways
Inflammation plays a central role in the development and progression of psoriasis. Inflammatory cytokines (proteins) produced by immune cells contribute to the skin inflammation and abnormal skin cell growth seen in psoriasis.
Abnormal Skin Cell Growth
In psoriasis, there is an imbalance in the normal process of skin cell turnover, leading to the rapid growth and accumulation of skin cells on the surface of the skin. This results in the characteristic thickened, scaly patches known as plaques.
Triggers and Exacerbating Factors
While not direct causes of psoriasis, certain triggers and exacerbating factors can worsen symptoms in individuals with existing psoriasis. These triggers can include stress, smoking, alcohol consumption, obesity, and certain medications.